Reconstructive surgery has long been admired worldwide for its incredible power to rectify abnormalities, restoring the body’s form and function. It involves the reshaping of traumatized features as well as congenital malformations through innovation and creativity. However, the methods, techniques, and materials employed for various reconstructive surgeries have evolved widely, thanks to the rapid advancement of surgical science and technology. While synthetic substrates are suitable for different surgical settings, they are getting replaced by biological choices like acellular dermis these days as they later integrate into the native tissue in a faster and better way. Alloderm is one of such biocompatible solutions that has revolutionized the approach to tissue expansion and reconstructive surgeries.
What Is Acellular Dermal Matrix (ADM)?
Before digging into the details of Alloderm, it is essential to be familiar with Acellular Dermal Matrices (ADMs). Introduced in 1994, they are biological scaffold materials used to augment or replace deficient or missing skin and soft tissues. The acellular dermis is typically derived from human or animal tissues processed for decellularization while keeping intact the structural element, i.e., extracellular matrix (ECM). This facilitates dermal scaffolding, which allows the repopulation and revascularization of the implanted tissue (1). Unlike traditional allografts and xenografts, this soft tissue matrix graft gets incorporated into the body in many plastic surgeries (reconstructive and cosmetic). In other words, it offers improved wound healing without the concern of rejection. Some of the most common ADMs available for reconstructive surgeons include AlloDerm, AlloMax, DermaMatrix, FlexHD, BellaDerm, Permacol, and Strattice.
Also Read – Get Rid Of Ugly Old Scars With Scar Revision Surgery
What is Alloderm?
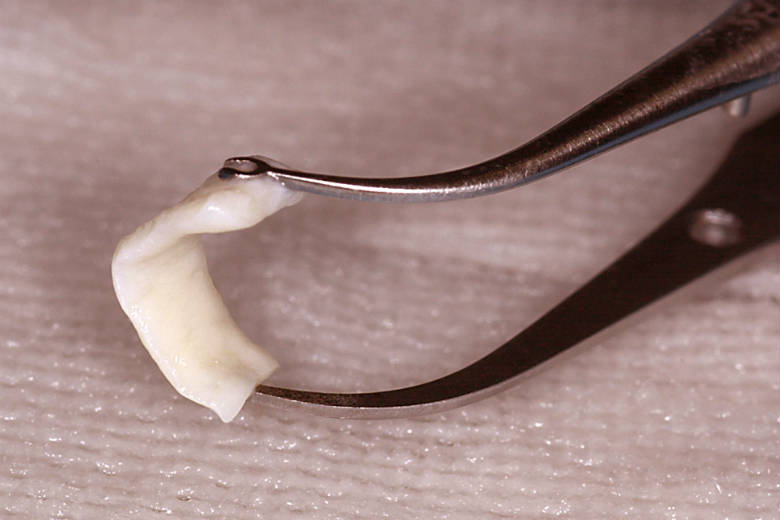
AlloDerm (a product by LifeCell Corp., Branchburg, New Jersey) is a regenerative tissue matrix with a uniform appearance and white to buff-color. It is one of the most widely studied and used ADMs harvested from donated (cadaveric) allograft human dermis. The dehydrated sheet of sterile tissue comes in different sizes and thicknesses to promote revascularization and cell migration. This stimulates natural tissue renewal and offers rapid wound healing with minimum limitations. The best thing about Alloderm is that it reinforces the compromised soft tissues in the body while ensuring lasting tensile strength and natural contour. Moreover, it fully integrates into the final wound without causing infection or extrusion.
Harvesting And Processing
The manufacturing of Alloderm is a multistep procedure that broadly includes explantation, decellularization, and sterilization. It is immersed in a buffered salt solution for separating and explanting the tissue from varying developmental stages of the human dermis; after that, all the cellular elements are removed by processing the tissue with mild detergents. Then, it is sterilized terminally to avoid contamination caused by infectious bacteria and viruses. Finally, the sterilized product is freeze-dried (lyophilized) on an intact basement membrane collected from donor skin to remove moisture and prevent crystallization. (2)
Also Read – African American Rhinoplasty – Procedure, Cost, Risks, And Complications
Regulatory Classification
Alloderm is approved by the US Food and Drug Administration (FDA) as banked human tissue for various clinical indications. It also fully complies with the Standards for Tissue Banking of the American Association of Tissue Banks (AATB) and applicable state requirements.
Is AlloDerm Safe?
To ensure the safety of Alloderm for transplantation, the U.S. Tissue Bank performs rigorous donor screening and testing. These include a host of steps, such as physical examination, interview for risk assessment, laboratory testing, and autopsy. An eligible donor should be negative for infectious diseases like HIV 1 and 2, hepatitis B and C, syphilis, etc. The tissue grafts are also tested to rule out contamination.
Who Are The Best Candidates?
An ideal candidate for Alloderm needs repairing or replacement of damaged integumental tissue.
Different Applications Of Alloderm
Alloderm has been used in various reconstructive surgeries as the first choice of surgeons for more than 20 years. Following are the fields of application in which it holds a consistent record of outstanding results:
Burn Reconstruction
Treating burn contractures and traumatic skin loss is the most basic use of Alloderm. It is meshed (1:1), placed on the wound bed, and immobilized. The practice reduces the need for multiple reconstructive surgeries and regrafting while significantly enhancing the range of motion.
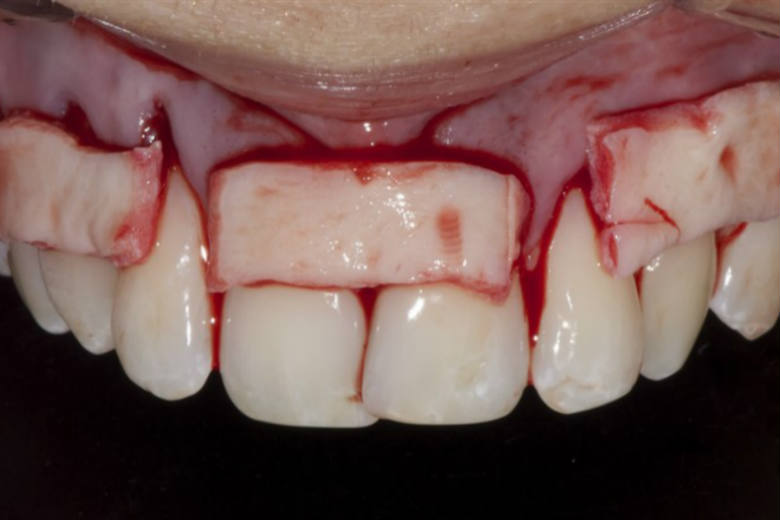
Gum Recession Treatment
Alloderm reverses the process of recession and restores the gum line successfully. This gives superior aesthetic outcomes and prevents severe oral issues like tooth root sensitivity, plaque and tartar build-ups, cavities, damage of supporting bone, etc.
Also Read – How To Smile Again Beautifully With All-On-4 Dental Implants
Dorsal Nasal Augmentation
In secondary rhinoplasty, the alloderm replaces the autogenous cartilage to expand portions of the nasal skin envelope with sufficient structural support and no unsightly irregularities over time. It helps maintain a soft natural contour while eliminating the risk of donor-site problems.
Breast Reconstruction
For implant-based breast reconstruction or corrective breast augmentation, Alloderm acts as internal support with excellent coverage. High in elastin, it has great stretchability that helps create a smooth contour by masking rippling and averting implant migration.
Besides these, Alloderm is frequently used in eyelid and periorbital surgery, cleft palate surgery in children, nasoalveolar bone grafting, tarsal plate reconstruction, diabetic foot ulcer treatment, etc.
How To Use Alloderm
Alloderm is used as a sheet during reconstructive surgeries. The sheet is shaped, rehydrated (using warmed and sterile saline solution), and implanted with the help of absorbable sutures. Each sheet has two sides – basement membrane or upper surface (repels blood) and dermal or lower surface (absorbs blood). The dermal side is typically placed against the most vascular tissue when applied as an implant. However, in a grafting procedure, it is placed against the wound bed with the basement membrane facing up.
What To Expect After Application
Just like any other cosmetic procedure, the application of Alloderm also results in redness, swelling, and mild bruising. But these are temporary and will subside within a few days. For the next 2-3 weeks, you must not get involved in any activity that interferes with the recovery and the growth of new tissue.
Recovery And Downtime
The healing time after Alloderm application varies based on the type of procedure performed. Though you can return to your routine within 7-10 days, the complete recovery can take a few months.
Adverse Reactions
Some common risks associated with Alloderm are allergies, hypersensitivity, wound or systemic infection, dehiscence, seroma, failure of the graft, etc.
Cost Of Using Alloderm
Multiple factors are taken into consideration to determine the total cost of Alloderm. These include the size of the sheet, the extent of damage to be repaired, the type of surgery to be performed, etc. Hence, it can range from $3,000 to $12,000 on average.
Summary
Reconstructive surgery has advanced with acellular dermal matrixes (ADMs) and biological scaffolds replacing synthetic materials. One prominent ADM is Alloderm, sourced from the donated human dermis. Alloderm supports natural tissue renewal, integrates well, and speeds up wound healing. It is applied in burn reconstruction, gum recession treatment, dorsal nasal augmentation, breast reconstruction, and other surgeries. Alloderm’s safety, harvesting process, regulatory compliance, and versatile applications make it a valuable tool in reconstructive surgeries, providing practical solutions for various medical needs.
References:
Acellular Dermal Matrix: General Principles for the Plastic Surgeon, Aesthetic Surgery Journal
Acellular dermis, Wikipedia